AHRQ Signals Intent To Fund Clinics To Improve Care for People With Long COVID
Issue Number
852
February 28, 2023
AHRQ Stats
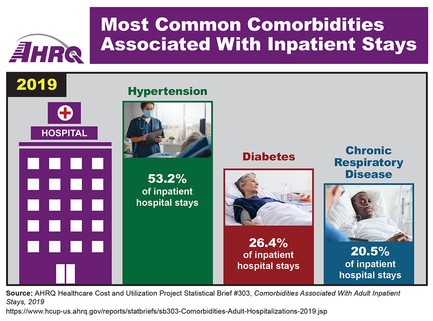
Access more data on this topic in the associated statistical brief, plus additional AHRQ data infographics.
Today's Headlines:
- AHRQ Signals Intent To Fund Clinics To Improve Care for People With Long COVID.
- Preventing Patient Falls Using an Evidence-Based Intervention May Reduce Costs.
- AHRQ To Host March 9 Webinar on Applications To Build Equity-Focused Evidence Base.
- Physicians Should Consider Potential Drug Interactions When Prescribing Colchicine.
- Highlights From AHRQ’s Patient Safety Network.
- Studies Highlight Patient Experience Survey Best Practices and Their Use Among Patient-Centered Medical Homes.
- AHRQ in the Professional Literature.
AHRQ Signals Intent To Fund Clinics To Improve Care for People With Long COVID
AHRQ plans to make up to $9 million available to support existing multidisciplinary Long COVID clinics to expand and improve care delivery. According to a recently published Notice of Intent, the agency will publish a Request for Applications in April or May that will call for proposals to expand access to comprehensive, coordinated and person-centered care for people with Long COVID, particularly underserved, rural, vulnerable or minority populations. Initiative goals include supporting new or improved care delivery models, providing services to more people, expanding services provided, strengthening care coordination and the implementation of best practices, and supporting the primary care community with Long COVID education and management. Awards will be made by Sept. 30, 2023.
Preventing Patient Falls Using an Evidence-Based Intervention May Reduce Costs
Implementing the AHRQ-funded Fall TIPS Program, an evidence-based fall prevention intervention, was associated with $22 million in savings at 33 medical and surgical units in eight hospitals, according to an AHRQ-supported study published in JAMA Health Forum. Researchers analyzed electronic health record data for 900,635 patients to identify the costs of fall-related adverse events on health systems. They found that the average total cost of a fall is $62,521 and that the level of injury was not a significant predictor of increased costs. After implementation of the Fall TIPS intervention, there was a nearly 20 percent reduction in falls and injuries at the study sites, and it was associated with $14,600 in net avoided costs per 1,000 patient-days. Policies to reduce all falls using evidence-based interventions could reduce the frequency of harms and associated costs. Access the abstract.
AHRQ To Host March 9 Webinar on Applications To Build Equity-Focused Evidence Base
AHRQ is seeking applications for research projects that will help build a new equity-focused evidence base to address disparities in healthcare delivery systems. The agency will invest up to $15 million over five years to help health systems transform care to be more equitable for patients, especially historically underserved populations. A technical assistance webinar will be held from 2 to 3 p.m. ET on March 9; advance registration is required. Grant applications are due April 21. Colleges and universities, including those serving minority populations, are strongly encouraged to apply, as are state and local governments and faith- and community-based organizations.
Physicians Should Consider Potential Drug Interactions When Prescribing Colchicine
Colchicine is medication to prevent and treat gout as well as other conditions, but it has potentially serious drug interactions that can cause adverse events like multi-organ failure and heart problems, according to two AHRQ-funded studies published in the Annals of Pharmacotherapy (AOP) and Drug Safety. The AOP study examined clinical outcomes associated with colchicine drug interactions using reports from the U.S. Food and Drug Administration’s Adverse Event Reporting System from January 2004 through June 2020. It found a total of 787 reports that pointed to an adverse event from a colchicine drug interaction. The Drug Safety study provided details on drugs known to interact with colchicine, as well as management options for reducing risk. Both studies emphasized that colchicine drug interactions can almost always be prevented through proper management and patient education.
Highlights From AHRQ’s Patient Safety Network
AHRQ’s Patient Safety Network (PSNet) highlights journal articles, books and tools related to patient safety. Articles featured this week include:
- Examining medication ordering errors using AHRQ network of patient safety databases.
- Assessment of patient retention of inpatient care information post-hospitalization.
- Defining and enhancing collaboration between community pharmacists and primary care providers to improve medication safety.
Review additional new publications in PSNet’s current issue or access recent cases and commentaries in AHRQ’s WebM&M (Morbidity and Mortality Rounds on the Web).
Studies Highlight Patient Experience Survey Best Practices and Their Use Among Patient-Centered Medical Homes
Two recent AHRQ-funded publications provide new insights into the use of patient experience surveys. A systematic review published in Medical Care found that mixed-mode data collection that combines web-based contact such as email with phone or mail follow-up can increase patient experience surveys response rates by five to nine percentage points. The review also found that phone surveys significantly improved responses among historically underrepresented groups. In another study published in the Journal of Ambulatory Care Management, researchers found that more than half of 105 aspiring or recognized Patient-Centered Medical Homes relied on AHRQ’s Consumer Assessment of Healthcare Providers and Systems Patient-Centered Medical Home survey to identify and improve patient experiences. While all aspiring practices were required to use some form of patient experience survey, over 70 percent chose to change the specific survey they use over time.
AHRQ in the Professional Literature
Evaluation of a fast-and-frugal clinical decision algorithm ('pathways') on clinical outcomes in hospitalised patients with COVID-19 treated with anticoagulants. Djulbegovic B, Hozo I, Lizarraga D, et al. J Eval Clin Pract 2023 Feb;29(1):3-12. Epub 2022 Oct 13. Access the abstract on PubMed®.
A sociotechnical systems framework for the application of artificial intelligence in health care delivery. Salwei ME, Carayon P. J Cogn Eng Decis Mak 2022 Dec;16(4):194-206. Epub 2022 May 11. Access the abstract on PubMed®.
The relationship between depressive symptoms, eHealth literacy, and asthma outcomes in the context of a mobile health intervention. Silverstein GD, Styke SC, Kaur S, et al. Psychosom Med 2023 Jan 27. [Epub ahead of print.] Access the abstract on PubMed®.
Designing and conducting scholarly quality improvement: a practical guide for improvers everywhere. Carroll AR, Smith CM, Frazier SB, et al. Hosp Pediatr 2022 Oct;12(10):e359-e63. Access the abstract on PubMed®.
i-CLIMATE: a "clinical climate informatics" action framework to reduce environmental pollution from healthcare. Sittig DF, Sherman JD, Eckelman MJ, et al. J Am Med Inform Assoc 2022 Nov 14;29(12):2153-60. Access the abstract on PubMed®.
Adoption of patient-reported outcomes by health systems and physician practices in the USA. Rodriguez HP, Kyalwazi MJ, Lewis VA, et al. J Gen Intern Med 2022 Nov;37(15):3885-92. Epub 2022 Apr 28. Access the abstract on PubMed®.
Integrating a patient engagement app into an electronic health record-enabled workflow using interoperability standards. Lobach DF, Boxwala A, Kashyap N, et al. Appl Clin Inform 2022 Oct;13(5):1163-71. Epub 2022 Dec 14. Access the abstract on PubMed®.
Pneumonia after hip surgery in children with neurological complex chronic conditions. Difazio RL, Shore BJ, Melvin P, et al. Dev Med Child Neurol 2023 Feb;65(2):232-42. Epub 2022 Jul 10. Access the abstract on PubMed®.



