Tools for Sustainability: Premortem and Scorecard: Facilitator Guide
AHRQ Safety Program for Mechanically Ventilated Patients
Slide 1: Tools for Sustainability: Premortem and Scorecard

Say:
This module will cover sustaining and spreading safety improvements. To preface the sustainability discussions, this module is designed to develop conversation and reflection on your safety program activities.
Slide 2: Learning Objectives

Say:
When a safety project is sustainable, the accomplishments are more likely to persist on the unit.
After this session, you will be able to–
- Define sustainment and spread.
- Plan key actions for sustainment.
- Prioritize needs for successful sustainment.
- Identify risks to sustaining your efforts with Premortem Tool.
- Design a scorecard with adaptive and technical indicators to measure performance as part of your sustainability efforts.
It’s critical to understand what sustainment and spread mean and why they different. During this module, consider the efforts at your unit or hospital and assess whether they are sustainable. The module provides you with tools to plan for sustainability in your intensive care area and prioritize actions for sustainability.
Slide 3: Sustainment Is...

Say:
Sustainability references the continual achievement of quality interventions in the context of culture of safety and quality improvement in your unit or hospital. It also refers to applying the process for improving care for mechanically ventilated patients to new challenges.
Slide 4: Adaptive or Technical?

Ask:
Now that sustainability has been defined, what parts of your quality improvement efforts will be tougher for you to sustain?
Say:
Often, teams believe that the tough work will be the technical side, or the ventilator-associated events prevention efforts. For example, teams often think that performing spontaneous breathing trials is hard. But technical work is concrete and backed by evidence-based literature.
Rather, it’s the adaptive or cultural components of this work that are not only the toughest to implement, but are also sometimes the tougher parts to entrench in your environment. The adaptive work of CUSP, the Comprehensive Unit-based Safety Program, involves everyone in your unit. Moreover, what works in one environment may not be successful in another area.
Slide 5: Why Worry About Sustainment?

Say:
Consider how to sustain your efforts as far in advance as possible. Recidivism, or the return to the previous way of doing things, hurts your sustainment effort. Especially if you have experienced positive momentum around safe ventilation initiatives, any backtracking can stall out that success.
Consider the barriers for sustaining team efforts. Take comfort from knowing that barriers are expected and that sustaining adaptive work is challenging. In fact, sustaining adaptive work has a high failure rate. This is due in part to overlooking cultural considerations. As you develop your sustainability plan, anticipate staff turnover at various levels in the unit or hospital. Also, consider the unit or hospital priorities and how they might compete with the improvement efforts in your clinical setting.
Slide 6: Definition of Spread

Say:
Due to competing priorities and organizational changes, people often rush into the next project or even spread an achievement into another area of the organization. But first consider what you’ve implemented and how strongly it’s become a part of the new way of doing things. If the process that you want to spread is still taking root, then dissemination may be futile.
Spreading takes the process from a narrowly segmented population and broadens it to include other populations. To do this successfully, formalize the new processes, as it provides a reference for new efforts. When sharing your accomplishments, talk about what you did, how you did it, and how you plan to sustain your efforts.
Slide 7: What Do Effective Teams Look Like?

Say:
In order to sustain and spread your initiatives, you need an effective team.
Effective safety teams have active members working for team goals. These teams meet regularly and communicate frequently. Most are honest about performance, including candid discussions about both barriers and successes. They enjoy active provider champions as well as the participation of an executive leader.
With active executive leadership support, many barriers can be mitigated. Most notably, effective teams believe that progress is possible. That is a huge component of whether or not the cultural psyche within the intensive care unit will continue to improve.
An effective safety team is diverse, with multiple disciplines represented, such as nurse managers, anesthesiologists, and respiratory therapists. Include ancillary departments like pharmacy and physical therapy. Diverse teams yield comprehensive solutions that are more likely to sustain safe care for mechanical ventilation efforts over time. An effective safety team excites staff members about doing this work.
Slide 8: What Sustainment Strategies Work?

Say:
Let’s turn to strategies that will help with the sustainability effort. The first is to stick to the formal processes. Continue to use the tools currently in place, such as your interventions, processes and structures. For example, the Daily Goals Checklist is a communication tool to share information learned during handoffs and rounding. Consider using this tool as a regular part of operations with multidisciplinary team members or within other clinical areas. Develop formal processes to sustain efforts, regardless of staff or management turnover. Reinforce these processes.
When proposing a new process, make sure to set up some early wins. Test the changes on a small scale before rolling out a new process. Gather data that verifies your proposed new workflow. For example, test a new tool with one provider on a shift or two. Recognize issues and modify the tool. Share the data with stakeholders that make decisions and use the tool. Require current data to validate progress.
Slide 9: What Sustainment Strategies Work?

Say:
It is important for people to know who is responsible for what, so formalize the roles and responsibilities on your safety team.
Ask:
Who will continue to schedule the meetings?
Who will share the meeting minutes?
Say:
Ensure all members of your team have a role. If there are resources, identify personnel and a funding source devoted to the mechanical ventilation safety effort by pitching this need.
Though project implementation may have an end date, that doesn’t mean the work ends. By clarifying what is expected, your diverse team can establish a new mode of operation.
Dedicated financial resources and personnel certainly help with sustainability. To continue to deliver on quality improvement efforts, your senior executive will need to support those efforts with resources and protected time. Data should drive your quality improvement efforts, so make data support available. In other words, identify who will have access to data and who will communicate data.
Make the data available for natural interaction. Ideally, data are available close to the bedside so that providers connect data with their daily actions.
Take care of your team. Listen to the frontline staff members and their suggestions. Be proactive about team turnover. Identify potential team members, including new practitioners, and invite them to join team meetings.
Recommend highly engaged team members attend professional development opportunities. Many will feel honored and appreciate the chance to bring more skills to their career and the team.
Slide 10: We Are Ready To Sustain: Now What?

Say:
We have defined sustainability and spread, described effective teams, and discussed applicable strategies. Here is a list of activities to sustain your efforts to improve care for mechanically ventilated patients.
Ask:
How do you think the next patient in your unit/clinical area will be harmed?
What can we do to prevent that harm?
How can we safely get the patient off the ventilator faster?
Say:
CUSP employs the Staff Safety Assessment or SSA, often called the two-question survey. The Safety Program for Mechanically Ventilated Patients has modified the tool for the acute care setting with an additional question: In your opinion, how can we get patients off the ventilator faster? Readminister the SSA at least every 12 to 18 months. Take the opportunity to listen to your frontline staff members and use the responses to prioritize the next activity.
Complete the Learning From Defects tool with your safety team for one defect per quarter. Select a defect, perhaps from your SSA responses. Walk through the four questions in the Learning From Defects tool:
- What happened?
- Why did it happen?
- How will you reduce the risk of the defect happening again?
- How will you know the risk is reduced?
Share the stories and results with your frontline staff. Even small wins help build momentum. Frontline staff members will feel a sense of accomplishment for their contribution to these exercises.
Ask:
What percentage of your current staff has viewed the Science of Safety video?
Say:
The Science of Safety video provides the basis for understanding the systems. It also highlights the difference between blaming people and recognizing the system factors
Slide 11: Sustainability and the Premortem

Say:
This section will cover Sustainability and the Premortem tool.
Projects can fail for many reasons, and improving care for mechanically ventilated patients is no exception to this possibility. Understanding barriers that can impede project implementation will help your team plan for the sustainability of your project’s achievements.
Slide 12: Problem Statement

Say:
Projects often fail due to many circumstances. This project is no exception. Understanding potential barriers to and complications of project implementation can help teams prepare to sustain improvements.
This module will walk through ways to identify those barriers. Generally, a premortem is conducted at the beginning of the project. This allows teams to reflect on how the project might fail before it starts and build in practices to prevent failure. In this section, the premortem exercise is framed to anticipate problems or barriers to sustainability.
The premortem is a step toward sustaining the mechanical ventilation safety initiatives in your unit. The idea is to brainstorm for possible failure points in order to address them.
Slide 13: Preparing To Lead
Say:
To better understand the premortem, consider the postmortem process. In the postmortem, the autopsy is performed to find out why the patient died. While that is helpful to the clinicians and those interested in the results, it doesn’t help the patient.
Slide 14: Preparing To Lead

Say:
Similarly, doing a postmortem for a project after it ends doesn’t help the functioning project. A premortem encourages you to imagine that the project has failed and brainstorm the reasons that could lead to this failure. After barriers to success are identified, develop plans to mitigate the barriers.
Work on this exercise as a team. If you complete the exercise individually, have team members share their responses with the team.
Slide 15: Preparing To Lead

Say:
The premortem exercise is used to identify potential barriers and vulnerabilities to long-term safe mechanical ventilation program successes. The successful use of this tool helps build team intuition for and sensitivity to future problems.
Projects fail when key stakeholders fail to speak up about their reservations during the planning stages. The premortem for sustainability focuses the safety team’s attention on the longevity of their intervention efforts. It allows the team to prepare a proactive approach to address those concerns.
There are four steps to completing the premortem exercise. The next few slides will review these four steps.
Slide 16: Premortem Exercise

Say:
The first step is to imagine that you’re 2 years into the future, and despite all of your best efforts, the mechanical ventilation safety program has failed.
Ask:
What might have gone wrong?
Say:
Let’s assume patient care hasn’t improved. Perhaps your team is not engaged. Maybe no one was available to gather data. Maybe no one has heard of your safety efforts.
In this first step, ask yourself what the worst-case scenario might look like.
Slide 17: Premortem Exercise

Say:
In step two, consider the reasons that caused your project to fail. Do this as a team. Brainstorm and document all of these reasons. Ask each team member what she or he thinks could go wrong.
Ask:
Was staff overburdened?
Were there too many competing priorities?
What could have caused our project to fail?
Slide 18: Premortem Exercise

Say:
In step three, identify the concerns that would be raised by each identified potential cause for failure.
Ask:
Is one more likely to derail your effort than another?
Say:
Which failures would impede sustainability of the safety program? Use the scale shown here to rank your team’s concerns about each failure.
Slide 19: Premortem Exercise

Say:
In step four, prioritize the list of reasons why your mechanical ventilation safety program could fail. Consider the concerns that you identified for each reason. Focus on the top two or three concerns that your group identified.
Ask:
What can your team implement to avoid or mitigate these failure points?
Slide 20: CUSP Premortem Summary

Say:
Here’s a summary of the steps in the premortem exercise:
- Two years after your safety program has started, what would the worst-case scenario for your efforts look like?
- What could have caused your project to fail?
- What specific actions can you take to avoid or manage these issues?
Review and anticipate potential problems throughout the project.
Conduct this premortem exercise with your team and share your insights at a followup meeting.
Slide 21: Discussion

Say:
When strategizing for sustainability, set goals for your sustainment.
Ask:
What elements of your mechanical ventilation safety program do you want to maintain?
Say:
Target potential risks for failure in order to achieve success in sustainment.
Remember that sustainment is more than a project; it is a process. Embed your sustainability plan into your system, and revisit as you move forward.
Slide 22: Discussion Questions

Say:
Discuss these questions with your team. The resulting conversation will help you plan for sustainability of your mechanical ventilation safety program.
Ask:
- What aspects of the project are you planning to sustain and how?
- What challenges do you predict for sustaining progress?
- How will you address these challenges?
Slide 23: Designing a Scorecard for Sustainability

Say:
This section covers how to design a scorecard for sustaining your mechanical ventilation improvement efforts.
Slide 24: Action Plan

Say:
This section continues the previous conversations about learning from defects. When the Learning From Defects tool was shared from the perspective of sustainability, teams were instructed to focus on learning from mistakes and problem solving at a deeper level.
The recommendation is to learn from at least one defect per quarter. Once your team has a few wins, consider participating in acute care setting conferences. Post the stories of the reduced risks, along with your data within your hospital network. Share stories of how defects were identified and what was learned from them. Celebrate successes with your teams.
Slide 25: Checking Your Progress

Say:
It’s important to take stock and check your progress. Strive to create collective awareness of team progress. Positive reinforcement is integrated by celebrating the things that are going well and what makes your team strong and effective. Tackle any remaining barriers or any barriers as they come up proactively rather than reactively.
Slide 26: Scorecard Parameters

Say:
Now let’s discuss some ideas about what to include in your scorecard. Rather than provide an established scorecard template, we recommend a flexible model with room for local customization.
As a starting point, we have listed some variables that are good indicators of long-term performance.
Ask:
How frequently are you meeting?
Say:
If your quality improvement team is no longer meeting regularly, it is difficult to achieve goals. If your team has lost momentum, consider revisiting your meeting schedule.
Ask:
Does your team have sufficient participation to facilitate your group goals?
Say:
The attendance patterns of specific participants in your team meetings can indicate team activity as well. If your provider champion rarely attends meetings, it may be difficult to meet physician needs and garner buy-in of other providers.
Ask:
How much of the staff has been trained in the Science of Safety?
Are you learning from each defect?
Are you keeping tabs on identified defects?
Is there a feedback loop for sharing progress on quality work?
Is staff turnover impacting your progress?
Say:
The last item covers safety culture. Though safety culture requires longer periods of time to change, pause to reflect on progress with data.
Ask:
How many safety climate responses are positive?
Does the staff know their concerns are being heard?
What is your response rate on safety culture assessments?
Slide 27: Sustainability Scorecard (Adaptive)
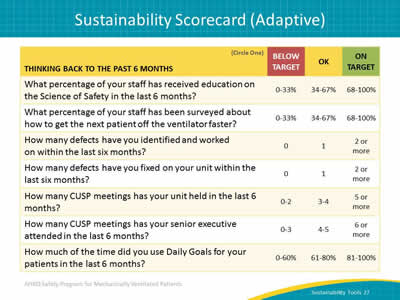
Say:
This template presents some adaptive elements, things related to teamwork and communication. As you create your scorecard, these categories may be useful.
The topic questions have been worded to fit a consistent schema: on target, OK, or below target. The score for each element indicates whether your team is above or below the desired goal. It signals where your team receives passing marks and where improvements are needed.
After you have recorded the number of team meetings held in the last 6 months, the dashboard columns score the results: Anything less than four is below target, maybe four in the last 6 months is OK, and five or six indicates you are on target.
Keep in mind that this is a guideline. For instance, colleagues impacted by harsh winter conditions may have been unable to attend some meetings. Adjust criteria to best fit your local expectations and needs. Regardless of circumstances, assessing the frequency of meetings provides an indicator for the health of your team.
Customize your scorecard to reflect your subgroup meetings as well. Several teams have reported two groups, such as daily care processes and early mobility groups. Recognize both how many subgroups meet and how often they are expected to meet on your scorecard.
The attendance questions ask who and how frequently specific team members attend meetings. Attendance and engagement are critical to success; perhaps an honest assessment about team member engagement will help determine if your team is optimally staffed.
Please note that senior executive attendance matters. A deputized stand-in is not a viable replacement for senior leadership engagement and consistent participation. Communication outside of safety meetings may be necessary to keep the senior executive informed and engaged.
Ask:
In addition to the senior executive, how many meetings did your provider champion attend in the last 6 months?
And your nurse champion?
Say:
Tailor your scorecard to fit your team members. For example, you can add other prominent roles represented on your safety team, like a respiratory or physical therapist.
Overall, the scorecard should help you reflect on the last 6 months. Design one that you can do collectively with your team every 6 months and assess a self-rating score on the health of your team.
For training, the Science of Safety training is the premier component of staff exposure to your team’s work efforts. Target at least 80 percent of staff to have viewed Science of Safety training within the last 2 years. Anything below 80 percent is below target. This is an example of a signal to determine how to get all staff members aware and involved.
Ask:
Have you embedded Science of Safety in onboarding or orientation programs for all new staff, including physicians?
Say:
Next, consider the defects that your team has addressed in the last 6 months. This section is intentionally ambiguous because defects come in a wide range of complexity. Some defects are quite simple to solve, while others could be as complex as a sentinel event requiring organization-level interventions.
Ask:
How many defects have you learned from in the past 6 months?
Say:
Each team should learn from at least one defect per quarter, including addressing contributing factors with interventions. It would be even better if your team has three defects solved in a quarter.
Ask:
How many of your improvement goals to address defects are data driven?
Some defects may not have data associated with them, but generally, the majority of defects do have supporting data. Present that data to the frontline providers and anyone impacted in those defects.
For safety culture assessments, review your average percent safety score. An acceptable target range is 60 percent to 80 percent, and scores greater than 80 percent are excellent. But anything below 60 percent indicates a red flag. Examine the low scoring domains to determine what is happening in that clinical area.
Ask:
For local safety culture, what is the unit response rate? Or what percentage of staff members completed safety culture surveys?
Say:
The higher the unit response rate is, the more representative the safety scores are to that clinical area. We often find that physicians complete fewer surveys than those in other job roles. If you find a role underrepresented in the survey, plan how to engage those groups in completing the survey.
Slide 28: Sustainability Scorecard (Technical)
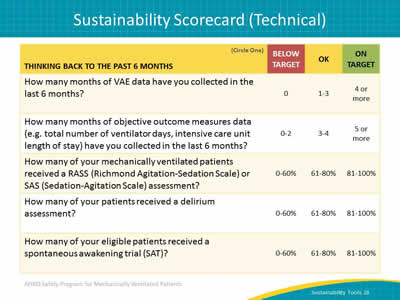

Say:
This scorecard provides an opportunity to evaluate technical processes and outcome indicators for your clinical setting. You can include indicators that would be applicable and relevant to your frontline clinicians.
The examples shown include months of ventilator-associated event data collected, and compliance with process measures, such as delirium assessment or spontaneous awakening trials.
Slide 29: Sustainability Scorecard (Technical)
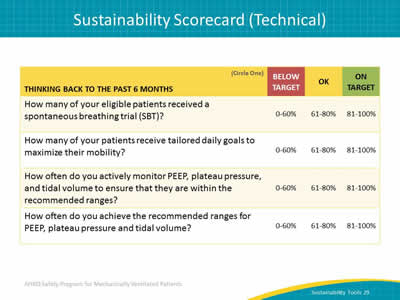
Say:
Additional examples include spontaneous breathing trials, daily goals for patient mobility, and monitoring of low tidal volume ventilation elements.
Slide 30: Keeping an Eye on Culture

Say:
Be aware of local performance using data, including understanding your most current safety culture responses and trends.
If you administer a culture survey to your staff regularly, use the comparative data points to recognize growth. Debrief the results with frontline staff and unit leadership. Use the safety culture improvements to validate the work efforts of your frontline staff.
Slide 31: Nurture Your Safety Culture

Say:
Throughout most of his life, 19th-century French chemist Louis Pasteur insisted that germs were the cause of disease, not the body. It wasn't until Pasteur was nearing the end of his life, having suffered multiple strokes before contracting pneumonia, that he reversed his perspective on the environment of the infection, reportedly saying, "It is the soil, not the seed."
In other words, a germ (the seed) causes disease when our bodies (the soil) provide a hospitable environment. In patient safety, the quality of the environment (the safety culture) greatly influences the safety of patient care. Nurture the safety culture; it is the environment for every interaction and intervention.
Slide 32: Questions

Ask:
Does anyone have any questions?
Slide 33: References




