Cultivating Leaders of Patient Experience Improvement
Many healthcare organizations are highly resistant to change. Employees may not be encouraged to solve problems on their own or to challenge the status quo. Many are accustomed to following standard operating procedures even when the policies and procedures may seem ineffective and outdated. Given the life-and-death issues confronted every day in most healthcare organizations, this risk-averse behavior is neither surprising nor hard to understand. This culture has grown even more challenging in the wake of the COVID pandemic, during which “command and control” management became paramount.
Because of this pervasive top-down culture, the search for better solutions and creative new approaches to longstanding problems requires strong and consistent encouragement and support. In order to achieve better patient experience, healthcare organizations must cultivate strong leaders throughout their organizations. Ideally, all levels of staff in the organization should become adept at leading change, making changes, and managing change.
What defines a leader?
Leaders are those who can:
- Communicate a compelling vision.
- Motivate clinicians and other staff to lower their resistance to change.
- Effectively and willingly participate in the redesign of new systems of care.
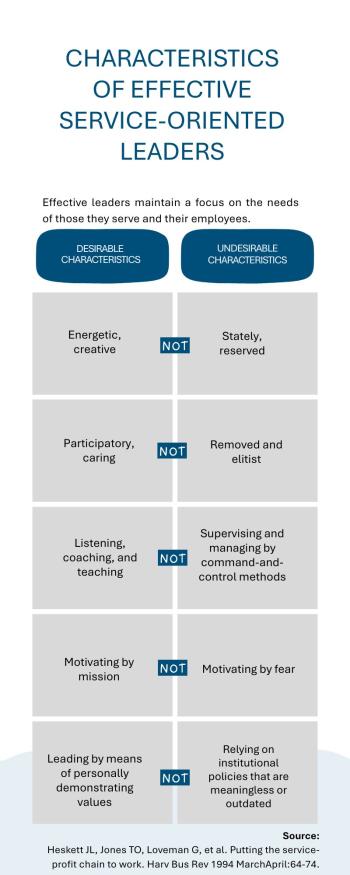
Sources of Leadership
Leadership for quality improvement (QI) can emanate from multiple parts of an organization: the CEO and senior leadership team, managers and frontline clinicians and staff, and the board. Leaders may obtain their power from the authority of a title, through mastery of knowledge, or through the strength of personality or persuasive abilities.
Senior leadership: Studies suggest that leadership from the top is a key factor in determining whether clinicians and others support and participate in QI efforts.1 Senior leaders set the tone and establish the policies and organizational structure that can either strengthen or undermine QI efforts. Chief Experience Officers play a critical role in setting the goals, identifying resources for improvement, and supporting improvement activities.
Managers and frontline clinicians and staff: The success of efforts to improve patient experience often depends on the involvement—or at least cooperation—of clinicians, administrative managers, nurses, other clinicians, and practice staff.2 Medical and administrative directors can also encourage cross-functional improvements by selecting interdisciplinary team members and physicians with a special interest in QI.
The board: Finally, strong board leadership can play a crucial role in QI. With the high turnover rates in healthcare senior executives, the board can help sustain a corporate culture focused on quality and provide “constancy of purpose.”3
Key Tasks for Leaders at Every Level
Those who study effective leadership have identified 10 practices that leaders at all levels can implement to produce and maintain an environment that emphasizes and encourages quality improvement:4
- Link QI goals to the organization’s mission and strategic plan (in other words, integrate improvement planning with business planning).
- Communicate the mission and values of the organization.
- Adopt and encourage a view of the organization as a system.
- Use measurement and management’s attention to keep the organization focused on the goals of QI efforts.
- Allocate financial and other resources (e.g., staff) to QI endeavors.
- Align incentives and performance appraisals to stimulate QI. (Learn more in: Recognizing and Rewarding Success in Delivering Better Patient Experiences.)
- Design and manage a system for gathering improvement information.
- Identify and remove barriers, which could be a function of finances, policies, system failures, internal politics, unsuitable attitudes, or legitimate concerns of personnel.
- Become directly involved in continuous improvement projects, perhaps by managing individual and team improvement activities.
- Market and advertise the QI work to the board, staff, and community through interpersonal communication, internal websites, social media, and other means.
While some of these activities may be more appropriate for senior leaders, most can be applied throughout the healthcare organization.
![]() Read about leadership
Read about leadership
- Committee on Military Trauma Care's Learning Health System and Its Translation to the Civilian Sector; Board on Health Sciences Policy; Board on the Health of Select Populations; Health and Medicine Division; National Academies of Sciences, Engineering, and Medicine; Berwick D, Downey A, Cornett E, editors. A National Trauma Care System: Integrating Military and Civilian Trauma Systems to Achieve Zero Preventable Deaths After Injury. Washington (DC): National Academies Press (US); 2016 Sep 12. 7, Leveraging Leadership and Fostering a Culture of Learning. Available from: https://www.ncbi.nlm.nih.gov/books/NBK390339/
- Berwick DM. A primer on leading the improvement of systems. Br Med J 1996;312:619-22.
- Berwick DM, Nolan TW. Physicians as leaders in improving health care. Ann Intern Med 1998;128:289-92.
- Lee YSH, Cleary PD, Nembhard IM. Effects of Leader Tactics on the Creativity, Implementation, and Evolution of Ideas to Improve Healthcare Delivery. J Gen Intern Med. 2021 Feb;36(2):341-348.
- Leebov W. Essentials for great personal leadership: No nonsense solutions with gratifying results. American Hospital Association. Chicago: Health Forum; 2008.
1. Weiner BJ, Shortell SM, Alexander J. Promoting clinical involvement in hospital quality improvement efforts: The effects of top management, board, and physician leadership. Health Serv Res 1997;32(4):491-510.
2. Alexander C, Tschannen D, Argetsinger D, Hakim H, Milner KA. A qualitative study on barriers and facilitators of quality improvement engagement by frontline nurses and leaders. J Nurs Manag 2022 Apr;30(3):694-701. doi: 10.1111/jonm.13537. Epub 2022 Feb 6. PMID: 34969172.
3. Weiner BJ, Shortell SM, Alexander J. Promoting clinical involvement in hospital quality improvement efforts: The effects of top management, board, and physician leadership. Health Serv Res 1997;32(4):491-510.
4. Langley GJ, Nolan KM, Norman C, et al. The Improvement Guide: A Practical Approach to Enhancing Organizational Performance. San Francisco: Jossey-Bass; 1996.



